By Daily Nation
Slightly over two years ago, just hours from when 2019 was going to segue into 2020, international news was awash with news of a new virus with flu-like symptoms spreading across China.
It was easy to ignore the sporadic pneumonia cases that were being reported in China’s Hubei province given that the Asian country has over the years been a fountainhead of zoonotic diseases (infectious diseases that are transmitted from animals to humans) like SARS, H5N1 bird flu, and H7N9 bird flu.
Fast-forward to 2022. We are now ushering in the third year of the Covid-19 pandemic with new hope and scare. For starters, towards the end of last November, the World Health Organization (WHO) named and categorised Omicron as a variant of concern. For a virus to be classified as a variant of concern, scientists check for three things: Whether the variant is more transmissible, causes severe disease compared to existing variants, or escapes immunity developed either naturally from infection or vaccination.
But 2022 is starting on a high when the world holds hope for an effective and widely available treatment for Covid-19 that would be a significant breakthrough for managing the pandemic.
Until now, the world has been relying on only therapies that have shown benefit before patients need hospitalisation or are at risk of dying. These are antivirals such as remdesivir (Veklury), monoclonal-antibody treatments, and vaccines. All these are given through a needle in the skin (intravenously), making them not only scarce but also very expensive.
“These (therapies) are impractical because they must be administered in a healthcare setting by injection,” observed Ilan Schwartz, an infectious-diseases physician at the University of Alberta Hospital in Edmonton, Canada.
Some drugs, however, have failed the test. To begin with, Ivermectin, a highly popularised drug despite scientists warning against its use, was never approved for treatment or prevention of Covid-19. Taking large doses of this drug can cause serious harm. Similarly, authorisation for the use of Hydroxychloroquine and chloroquine in Covid-19 treatment was withdrawn after data analysis showed that the drugs are not effective for treating the virus.
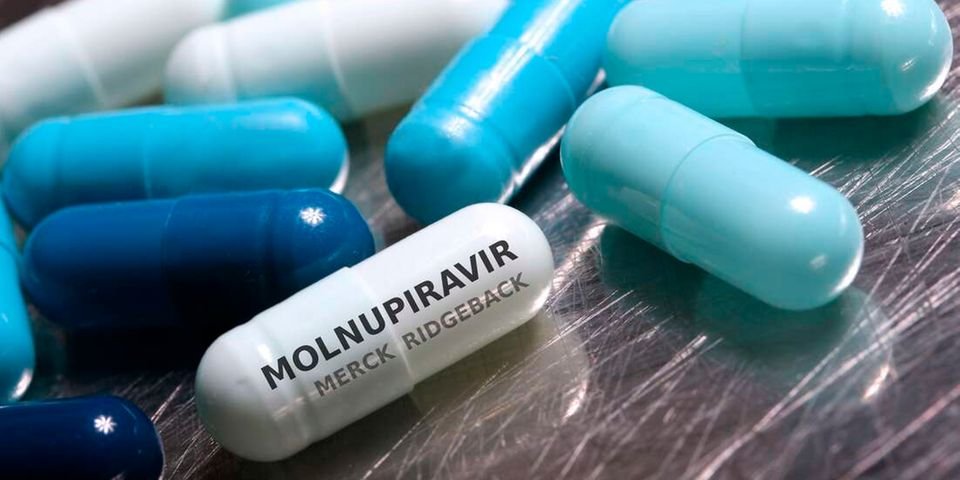
However, in recent months, research has found that three drugs: Paxlovid from Pfizer, Molnupiravir from Merck and Ridgeback Biotherapeutics, and Fluvoxamine, a pill originally approved in 1994 to treat obsessive-compulsive disorders and often prescribed off-label for anxiety, depression, and panic attacks, are effective in the management and treatment of Covid-19 when administered early.
“We still have lots to learn about how effective these medications are against Covid-19 but at least we can say that they are genuinely promising,” said Jeremy Faust, an emergency medicine physician at Brigham and Women’s Hospital in Boston and an instructor at Harvard Medical School.
Late last month, two oral antiviral medicines for the early treatment of Covid-19 were authorised in the US. The pills, Paxlovid and Molnupiravir, were authorised by the US Food and Drug Administration (FDA). The pills, taken by mouth, could be a game-changer for people considered at high risk of developing serious illness because they can be taken at home twice a day for five days to prevent hospitalisation and death.
On the same day the Pfizer treatment was authorised, a study on remdesivir published in the New England Journal of Medicine found that the three-day antiviral is highly effective at avoiding hospitalisation and death if given early in the course of illness.
For this category of people, Paxlovid was found to be 89 per cent effective when taken within the first three days of symptoms and 88 per cent effective when taken every 12 hours for the first five days. Paxlovid includes nirmatrelvir – a drug that blocks the activity of a specific enzyme needed for the virus that causes Covid-19 to replicate – and an antiviral drug called ritonavir that helps slow the breakdown of nirmatrelvir.
Molnupiravir, initially developed for the treatment of influenza, has been approved to treat mild to moderate Covid-19 in adults who are at higher risk of serious illness and who are not able to take other treatment options. But it is not authorised for use for longer than five consecutive days. The treatment will be more widely available at first, but it reduced hospitalisation by only 30 per cent among high-risk patients. It is only meant for adults because it could interfere with bone and cartilage growth in children. It is also not recommended for pregnant people because animal studies showed there could be some effects on the fetus. Men who want to start a family should wait for 90 days after the treatment.
“This drug works by introducing mutations and errors in that replication of the genetic material, and the concern is that it could potentially be the same thing for replication of genetic material in gametes, or sperm and new embryos,” said Peter Anderson, a professor of pharmaceutical sciences at the University of Colorado.
According to Patrizia Cavazzoni, director of the FDA’s center for drug evaluation and research, Molnupiravir is limited to situations where other FDA-authorised treatments for Covid-19 are inaccessible or are not clinically appropriate and will be a useful treatment option for some patients with Covid-19 at high risk of hospitalisation or death.
In studies, scientists have found that fluvoxamine is highly effective at preventing hospitalisation in Covid-infected patients.
Molnupiravir and Paxlovid have received approval in several countries like the US, UK, Denmark, and the Philippines; and 15 countries have gone ahead to place orders of large quantities of either drug.
Given an estimated time of six to eight months to ramp up production and with Pfizer expecting to make 120 million courses of the treatment in 2022, it might once again take longer for low-and middle-income countries to acquire the pills.
And just like the vaccines, the availability of the drugs comes with some significant caveats, including the fact that supplies of the Pfizer treatment are very limited, while the Merck treatment is less effective than hoped.
“Through sub-licensing agreements, Merck has committed to making the drug accessible globally with manufacturers around the world to provide at a reduced cost,” notes Dr Schwartz.
Further, access to timely treatment will be an issue, compounded by the fact that the drugs will only be available by prescription from a doctor or health worker, limiting those who can get hold of it.
And the pills are not for everyone.
Both treatments will be given only to people at high risk of being hospitalised or dying from Covid-19, similar to the populations studied in the clinical trials. The Merck treatment will not be given to children or pregnant women. Pfizer’s pill (Paxlovid) is not recommended for people with liver or kidney issues and has the potential to cause other medications to work differently during the treatment course. Beyond supply, Paxlovid has been found to have a drug-to-drug interaction with certain ones like some heart medications and blood thinners, for example.
Safe and effective treatments for early phases of Covid-19 in patients who are not yet requiring hospital care have been a persistent gap in the pandemic. Should we hold our breath about them?
“There is a reason for optimism with respect to molnupiravir (though we haven’t seen enough data) and fluvoxamine. But I doubt either of them is “the answer” we have all been looking for; neither is it just a pill that we can all take and, voilà, no more pandemic. I think they are both likely to help a subset of patients in a meaningful and measurable way. That is important, but I do not want to overstate it. Far better to never get sick in the first place. The best way to achieve that is via vaccines,” says Dr Faust. “Overall, I am optimistic about fluvoxamine because we now have two randomised trials, the 2nd of which was reasonably sized. My main pause is that some of the outcomes we care about weren’t different when you assess the data in the most rigorous ways.”
Lancelot Pinto, a consultant respirologist at P.D.Hinduja National Hospital and Medical Research Centre, India explains: “Drugs such as Ivermectin and Hydroxychloroquine never really had any high-quality evidence to support their use. However, at the start of the pandemic, when there was little known about the disease, they were tried as experimental therapies, and small observational trials which were often highly biased, reported some success. In India, a drug called Favipiravir, which was approved based on a study that had 150 patients and did not meet the primary end-point, ended up being used rampantly, despite being ineffective and expensive.”
Experts are concerned the virus could evolve to be resistant to these treatments, as has happened with some monoclonal antibodies and, in one study, remdesivir. Giving a mix of different drugs, instead of just one kind of antiviral, would probably prevent resistance, they add.
“If at-risk people are able to access the treatments quickly before the virus has a chance to take hold, you can basically shut down replication,” says Dr Ahmed Kalebi, a Nairobi-based consultant pathologist.
Lately, public interest in medical research has been dominated by treatments and vaccines for Covid-19. But the pharmaceutical industry is also focusing to develop new treatments and therapies for other diseases like haemophilia, brain disorders, HIV/AIDS, and malaria.
In December, the US FDA announced its first approval of a long-acting HIV prevention medication known as cabotegravir, making it the first injectable Pre-exposure prophylaxis (PrEP). PrEP is the use of HIV medication by people who do not have HIV to prevent infection.
Developed by ViiV Healthcare, cabotegravir injected once every two months was found to be superior when compared with traditional PrEP regimens. Currently, PrEP tablets like Truvada and Descovy are available for use.
In December, the Board of Gavi, the Vaccine Alliance, approved an initial investment of US$ 155.7 million (about Sh17.7 billion) for 2022-2025, which will initiate the implementation of malaria vaccine RTS,S, known by the brand name Mosquirix. It requires four injections.
The year 2022 will also see giant strides made in treating haemophilia, an inherited genetic disorder that impairs the body’s ability to make blood clots, a process needed to stop bleeding, which has been with humanity throughout history and now affects an estimated 1.1million men around the world.
In June 2021, the FDA approved the first Alzheimer’s drug since 2003. Aducanumab, under the brand name Aduhelm, is meant to treat Alzheimer’s, a progressive disease that destroys memory and other important mental functions.
A majority of non-opioids development is similarly underway for pain management. Globally, about 0.5 million deaths are attributable to drug use, according to WHO. More than 70 per cent of these deaths are related to opioids, with more than 30 per cent of those deaths caused by overdose.
Opioids have analgesic and sedative effects and are commonly used for the management of pain.
According to the World Drug Report 2018, the non-medical use of prescription medicine is becoming a serious threat to public health and law enforcement. Opioids accounted for three in four deaths where drug use disorders were implicated.
Researchers are studying other potential treatments for Covid-19, including
• Antiviral drugs: In addition to remdesivir, other antiviral drugs being tested include favipiravir and merimepodib. Studies have found that the combination of lopinavir and ritonavir isn’t effective.
• Dexamethasone: Studies have found that it reduces the risk for deaths by about 30 per cent for people on ventilators and by about 20 per cent for people who needed supplemental oxygen. The drug is now being used for people hospitalised with Covid-19 who are on mechanical ventilators or need supplemental oxygen.
• Anti-inflammatory therapy: Researchers are studying many anti-inflammatory drugs to treat or prevent dysfunction of several organs and lung injury from infection-associated inflammation.
• Immune-based therapy: The use of a type of immune-based therapy called convalescent plasma was highly popularised for early treatment of Covid-19 but was found not to be very effective along the way.